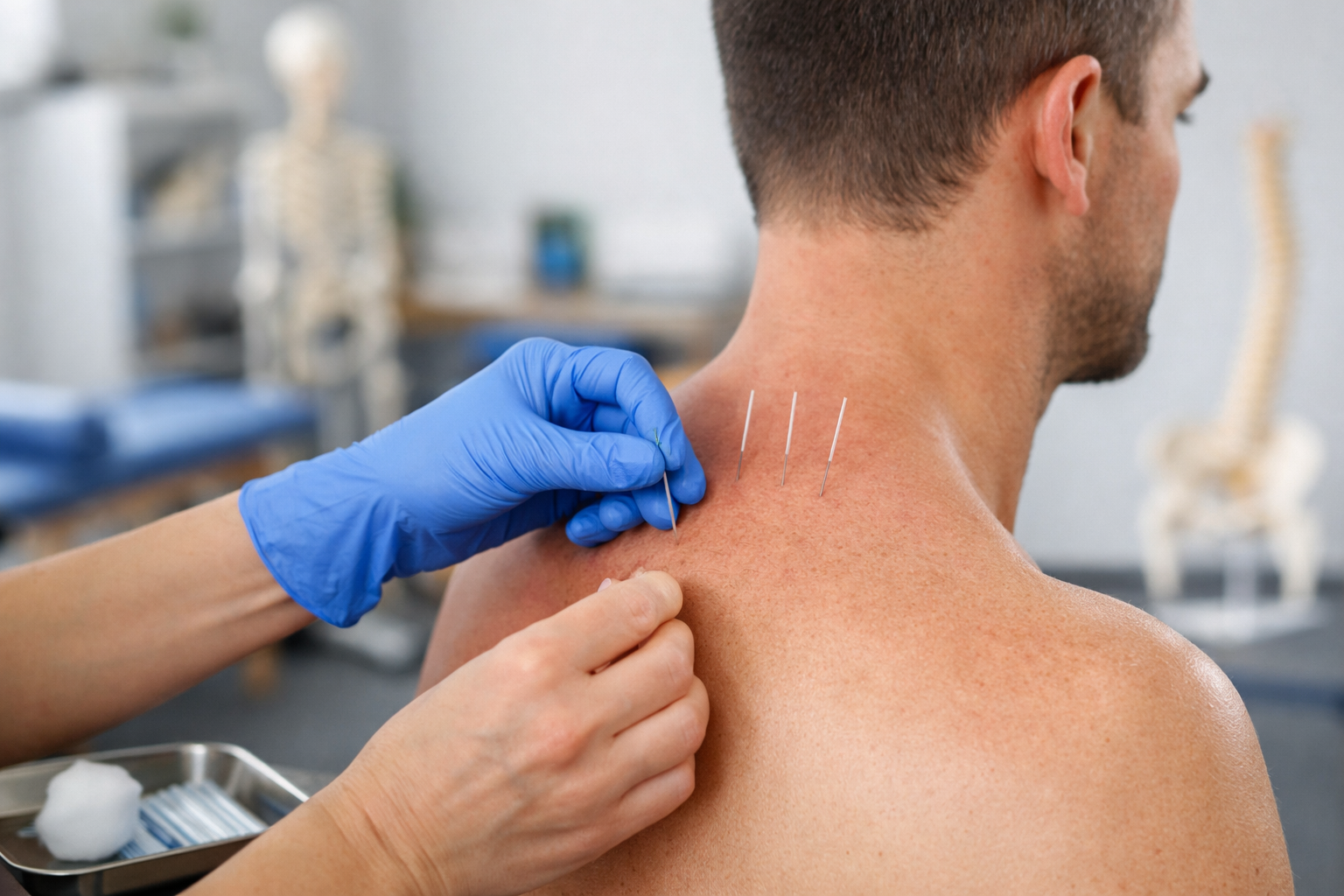
What Is Dry Needling?
(How it works, what it helps, and what to expect)
(Updated February 2026)
Dry needling is a modern technique physical therapists use to reduce pain, improve mobility, and help patients tolerate exercise and rehab more comfortably. It involves inserting a very thin, solid needle into sensitive muscle or connective tissue points—often called “trigger points”—to decrease tension and improve function.
Dry needling is not a standalone “magic fix.” The best results usually come when it’s used as a tool alongside a progressive rehab plan (strengthening, mobility, and movement retraining).
Dry needling vs acupuncture: what’s the difference?
Both use thin needles, but they’re based on different frameworks:
-
Acupuncture is rooted in Traditional Chinese Medicine.
-
Dry needling (in PT) is typically based on modern anatomy, neurophysiology, and pain science, and is used to address neuromusculoskeletal pain and movement limitations.
What does dry needling help with?
Dry needling is most commonly used for myofascial pain—pain related to muscle sensitivity and trigger points—and is often applied to:
-
Neck pain with trigger points
-
Low back pain with muscle-related sensitivity
-
Shoulder and upper back tightness
-
Headache patterns that have a muscular component
-
Overuse and training-related muscle pain (when trigger points are involved)
Research summaries and systematic reviews generally show short-term improvements in pain and function for some conditions—especially where trigger points and myofascial pain are prominent (e.g., neck pain, myofascial low back pain).
Key point: It’s typically most useful when it helps you move better and tolerate loading—so you can actually progress your rehab.
How does it work?
Dry needling appears to work through a combination of effects, such as:
-
Reducing trigger point sensitivity and muscle “guarding”
-
Changing local pain signaling in the tissue
-
Modulating the nervous system’s sensitivity (the “alarm system”)
There’s still active research on exact mechanisms, but clinically, many patients experience:
-
Less “tightness” or grabbing pain
-
Better range of motion
-
Improved tolerance to strengthening exercises
What a session feels like
Most people describe dry needling as a quick pinch or cramp, sometimes followed by a brief twitch response in the muscle. Afterward, it’s common to feel:
-
Mild soreness (like a workout soreness) for 24–48 hours
-
Temporary bruising or tenderness in the area
That soreness is normal and usually manageable with light movement, hydration, and heat (if you tolerate it well).
How many sessions do people usually need?
It depends on the problem and the overall plan. Some patients notice meaningful relief quickly; others need a few sessions to calm down sensitivity while they build strength.
We generally use dry needling in a way that supports a bigger goal:
-
“Move better today”
-
“Train better this week”
-
“Progress the program over the next month”
Is dry needling safe?
When performed by properly trained clinicians, dry needling is generally considered safe, and most side effects are mild (temporary soreness, bruising).
That said, serious complications can occur rarely, especially if needling is performed in higher-risk regions (like the upper chest/neck area). Pneumothorax (collapsed lung) is the complication most people have heard about—it’s rare, but documented.
We prioritize:
-
Appropriate screening (history, risk factors)
-
Informed consent
-
Conservative technique selection
-
Using dry needling only when it fits the clinical picture and plan
Who should NOT get dry needling (or should talk to us first)?
Dry needling may not be appropriate—or may require extra caution—if you have:
-
A bleeding disorder or you’re on blood thinners (depends on medication/dose and region treated)
-
A compromised immune system or active infection
-
Pregnancy (especially certain regions/first trimester—case-by-case)
-
Significant needle phobia or fainting history
-
History of pneumothorax or significant lung disease (again, case-by-case)
Also: if you have new, unexplained symptoms (fever, unexplained weight loss, worsening neurological symptoms), you should be medically evaluated first.
Dry needling works best when paired with the right plan
At Quincy Physical Therapy, we use dry needling as a tool to support:
-
Orthopedic & Sports Physical Therapy (return to lifting, running, sport)
-
Low Back Pain Physical Therapy (reduce guarding so you can move + load again)
-
Chronic Pain Physical Therapy (when sensitivity is part of the picture, alongside education + graded exposure)
-
Manual Physical Therapy (when joint/soft tissue mobility limits movement)
-
Strength Training and Performance (progressive loading once symptoms calm)
If your pain started at work and needs documentation/coordination, we also integrate it into Workers’ Compensation Physical Therapy plans when appropriate.
FAQs
Does dry needling hurt?
It can be uncomfortable for a moment, but most people tolerate it well. A quick twitch response can feel intense briefly, then settles.
How will I feel afterward?
Most people feel mild soreness for 24–48 hours. Bruising can happen occasionally.
Is it the same as cortisone or an injection?
No. The needle is solid (no medication is injected).
Can dry needling “fix” my shoulder/back/neck pain by itself?
Usually it helps reduce symptoms and improve mobility, but lasting results typically come from the rehab plan that follows—strength, movement, and load tolerance.
Is there research supporting it?
Yes—there are systematic reviews and clinical trials showing dry needling can improve pain and function in certain conditions (especially myofascial pain presentations), often most clearly in the short term.
References
1) American Physical Therapy Association (APTA) — Dry Needling (overview)
https://www.apta.org/patient-care/interventions/dry-needling
2) Hernández-Secorún M, et al. (2023) — Effectiveness of Dry Needling in Improving Pain and Function in Chronic Neck Pain (meta-analysis) — PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC10469395/
3) Dach F, et al. (2023) — Treating myofascial pain with dry needling: systematic review for best evidence-based practices in low back pain — PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC10756779/
4) Pandya J, et al. (2024) — Dry Needling Versus Manual Therapy for Mechanical Neck Pain: Randomized Controlled Trial — JOSPT
https://www.jospt.org/doi/10.2519/jospt.2024.12091
5) Chys M, et al. (2023) — Clinical Effectiveness of Dry Needling in Patients with Musculoskeletal Pain: Overview of Systematic Reviews — PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC9917679/
6) Bontinck JSB, et al. (2024) — Pneumothorax as a complication of dry needling technique (case series) — ERJ Open Research
https://publications.ersnet.org/content/erjor/10/2/00156-2024
7) Federation of State Boards of Physical Therapists (FSBPT) — Dry Needling Competency Update: Report Memo 2024 (PDF)
https://www.fsbpt.org/Portals/0/documents/free-resources/DN%20Competency%20Update%202024%20-%20Memo.pdf